Belmont Private Hospital Launches TMS Outpatient Clinic
Due to the increased demand for Transcranial Magnetic Stimulation (TMS) Therapy, Belmont Private Hospital is excited to announce that we have extended our services by opening a dedicated outpatient clinic to offer increased access to the evidence-based and innovative therapy.
Delivered in a safe, easily accessible and non-invasive setting, the introduction of the TMS outpatient clinic will benefit a wide range of patients seeking increased access to treatment for medication-resistant depression and other mental health concerns.
Transcranial Magnetic Stimulation (TMS) is a non-invasive procedure that uses magnetic fields to stimulate nerve cells in the brain to improve symptoms of depression. It is typically used when other depression treatments have proven ineffective.
In research and clinical practice, it is found that more than half of patients who receive TMS treatment achieve complete remission from depressive symptoms and when combined with Psychotherapy and offers an enhanced benefit (see Donse et al. 2017).
TMS therapy has proven to be an effective treatment option for medication resistant depression. 58% of people who had already tried two antidepressants in relieving depression reported to experiencing remission of depression symptoms after treatment (see Donse et al. 2017).

TMS services across Healthe Care have implemented evidence based outcome measures to monitor efficiency of TMS treatment. The DASS 21 – Depression, Anxiety and Stress scale is a set of three self-report scales designed to measure the negative emotional states of depression, anxiety and stress.
Across Healthe Care, the DASS 21 scale has demonstrated prior to treatment patients self-reported extremely severe levels of depression with mild symptoms or complete remission following the completion of treatment.
Outcome measures of anxiety also indicate severe self-reported levels prior to treatment with a reduction to mild symptoms once treatment had been completed.
Stress outcome measures similarly show severe levels prior to treatment with mild symptoms following TMS intervention.
The Montgomery–Åsberg Depression Rating Scale (MADRS) is a clinical rated evidence based outcome measure which stratifies the severity of depression in adults. It has also demonstrated significant improvements that endorse patient reported DASS 21.
With an average score of 36 pre TMS treatment is indicative of severe depression and show post a course of TMS patients reported only mild residual symptoms.
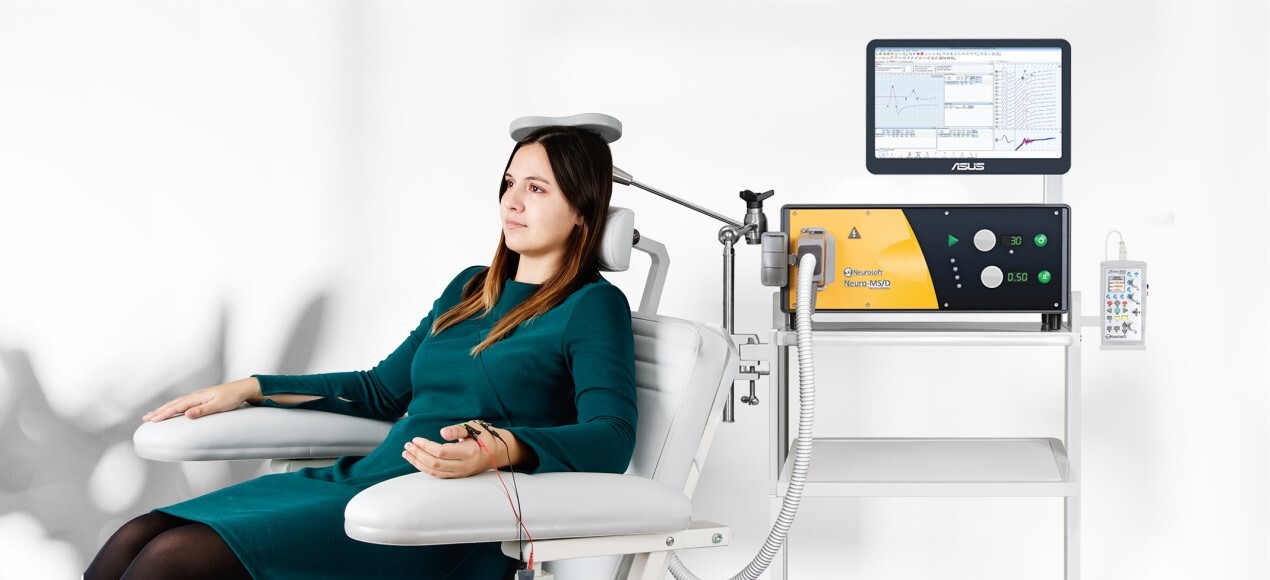
Belmont Private Hospital CEO/DCS, Mary Williams says the new clinic will enable patients to access TMS treatment in a more timely and affordable way.
“The commissioning of Belmont Private Hospital’s TMS Clinic will provide patients with an opportunity to obtain access to TMS in a more flexible treatment setting and in accordance with the principles of least restrictive care that guide mental health service delivery in Australia,” says Mary.
“Our vision is to continue to provide a comprehensive suite of private mental health services to our local community. I look forward to expanding these service offerings with the establishment of Belmont Private Hospital’s TMS Clinic.”
To access Belmont Private Hospital’s TMS Clinic, a referral from a General Practitioner or Psychiatrist will be required. If the referring Psychiatrist is not credentialed to provide TMS at the Outpatient Clinic, an initial assessment will be required.
To learn more about TMS therapy and our newly introduced outpatient clinic:
- Visit the TMS Clinic at Belmont Private page
- Contact our dedicated Admissions and Assessment team by phoning 1800 700 274.